SPECIAL SERIES: COMORBIDITY ACROSS THE COUNTRY
This review is the third in a series of five issues of the BASIS featuring the most recent research on comorbidity among psychiatric and addictive disorders. In the past two weeks, The WAGER and The DRAM have discussed findings from the National Epidemiological Survey on Alcohol and Related Disorders and the National Comorbidity Survey Replication about psychiatric and personality disorders comorbid with pathological gambling and alcohol use disorders. This week, ASHES discusses findings from the original National Comorbidity Survey on the relationship between of smoking and psychiatric disorders.
Smoking often co-occurs with mood and anxiety disorders as well as other addictive behaviors. Recent studies have provided a variety of explanations for this co-occurrence including the anxiety-producing effects of nicotine (Parrott, 1999), fear of developing lung cancer (Breslau & Klein, 1999), or use of “gateway” drugs such as nicotine leading to the use of other substances (Kandel, Yamaguchi, & Chen, 1992). This week ASHES reviews a study by Breslau, Novak and Kessler (2004a) which investigates the relationship between daily smoking and the subsequent occurrence of psychiatric disorders.
The investigators used data from the National Comorbidity Survey (NCS), a collaborative investigation of the prevalence, causes, and consequences of psychiatric morbidity and comorbidity supported by the United States National Institute of Mental Health. The NCS collected data from a representative sample of 8,098 people ages 15 to 54 in the United States. This study was limited to 4,414 respondents in the NCS who completed the Tobacco Supplement questionnaire on tobacco use (e.g., ever smoked daily for a month or more, onset of daily smoking) and nicotine dependence. Lifetime prevalence of psychiatric disorders was assessed using a modified version of the World Health Organization’s Composite International Diagnostic Interview (CIDI), a structured interview designed to be administered by lay interviewers. Breslau et al. focus on 10 psychiatric diagnoses on which the CIDI has demonstrated good validity and reliability: major depression, dysthymia, panic disorder, agoraphobia, simple phobia, social phobia, generalized anxiety disorder, post-traumatic stress disorder, and alcohol and drug abuse/dependence.
The investigators used survival analysis to predict the onset of specific psychiatric disorders from daily smoking status (current versus past daily smoking), nicotine dependence, and years since quitting smoking. The authors argue that smoking can be identified as a causal factor for other psychiatric disorders only if daily smokers are at greater risk for the disorders than others and that risk decreases proportionately to the years since quitting.
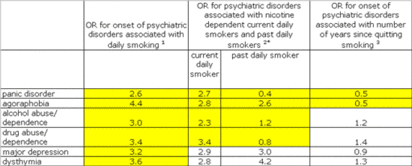
Figure. Associations between Daily Smoking and Comorbid Disorders (adapted from Breslau et al. 2004). Click image to enlarge.
Notes: Odds ratio (OR) are from a series of 10 survival models with non-daily smoking as reference Statistically significant associations (p < .05) are highlighted in yellow
* Patterns of statistical significance were the same for smokers who were not nicotine dependent
1 adjusted for sociodemographic characteristics
2 adjusted for sociodemographic characteristics and other pre-existing psychiatric disorders
3 adjusted for ever smoking, sociodemographic characteristics, and other pre-existing psychiatric disorders
The authors found that people who smoked daily at some point in their lives were significantly more likely to exhibit the disorders in the Figure (statistically significant associations are highlighted in yellow) than people who had not. The authors argue that the results show daily smoking is a causal factor for panic disorder and agoraphobia, since onset of these disorders is predicted by current smoking and risk of developing the disorders decreases for people who quit smoking. There is no evidence of a causal association between smoking and the other psychiatric disorders. However, the results show that current smokers’ risk of alcohol abuse/dependence and drug abuse/dependence is greater than past smokers’ risk for these disorders. Though not causally related according to the authors, daily smoking co-occurs with the onset of major depression and dysthymia, suggesting that these conditions share risk factors.
This study has several limitations. First, data on tobacco use and nicotine dependence are assessed retrospectively and, therefore, are subject to recall bias. Second, there was no year by year assessment of smoking, so periods of time without smoking could not be identified. Third, results may not be generalizable to all smokers because these results focus on daily smokers compared to people who do not smoke on a daily basis. More complete information about smoking behavior would be needed to analyze other patterns of smoking behavior.
If the authors’ conclusions are correct, these finding have important public health implications: interventions that target smoking cessation might also prevent the subsequent onset of panic disorder and agoraphobia, and active smoking might serve as a marker for preventing other substance use disorders. However, the authors do not address the possibility that people with subclinical levels of panic disorder and agoraphobia might use smoking as a form of self-medication to calm their nerves (Khantzian, 1990) as symptoms of these disorders begin to develop. If this were the case then smoking cessation programs might exacerbate rather than improve the symptoms of these psychiatric disorders. Alternatively, the implications to take away from these findings would be to treat the underlying subclinical symptoms of psychiatric disorders in smokers before these symptoms develop into full blown disorders. Further research on the associations between daily smoking and the subsequent onset of psychiatric disorders is needed to develop effective public health strategies to prevent smoking and the onset of psychiatric disorders.
–Allyson Peller.
References
Breslau, N., & Klein, D. F. (1999). Smoking and panic attacks: An epidemiologic investigation. Archives of General Psychiatry, 56(12), 1141-1147.
Breslau, N., Novak, S. P., & Kessler, R. C. (2004). Daily smoking and the subsequent onset of psychiatric disorders. Psychological Medicine, 34(2), 323-333.
Kandel, D. B., Yamaguchi, K., & Chen, K. (1992). Stages of progression in drug involvement from adolescence to adulthood: Further evidence for the gateway theory. Journal of Studies on Alcohol, 53(5), 447-457.
Khantzian, E. J. (1990). Self-regulation and self-medication factors in alcoholism and the addictions: Similarities and differences. In M. Galanter (Ed.), Recent developments in alcoholism (Vol. 8, pp. 255-271). New York: Plenum Publishing Corp.
Parrott, A. C. (1999). Does cigarette smoking cause stress? American Psychologist, 54(10), 817-820.
What do you think? Please use the comment link below to provide feedback on this article.





