Medication Assisted Treatment (MAT) is an effective approach to treating opioid use disorder (OUD), but not enough people have access to it, or use it when they do have access. Emergency medical services (EMS) personnel (e.g., firefighters and paramedics) are strategically positioned to link people to MAT, as they are often the first to respond to overdose events and provide immediate care. This week, STASH reviews an investigation by Christy K. Scott and colleagues into the feasibility of the Recovery Initiation and Management after Overdose (RIMO) intervention, which combines assertive outreach and linkage strategies — initiated by EMS workers — with recovery management checkups, to engage individuals in MAT following an overdose.
What was the research question?
What is the feasibility of a combined outreach and treatment-linkage intervention, initiated by EMS personnel following an overdose, on getting not-in-treatment individuals into sustained treatment for opioid use disorder?
What did the researchers do?
The researchers recruited thirty-three participants, all of whom had been administered naloxone by EMS personnel to reverse an opioid-related overdose within the past 30 days and were not currently engaged in any form of substance use treatment. EMS personnel informed participants about the study immediately following the overdose reversal and asked for permission to release participants’ contact information to the study team (i.e., linkage managers). Linkage managers then enrolled participants in the study, if eligible. Once enrolled, participants completed a baseline assessment and were randomly assigned to either the RIMO experimental group or the control group. Individuals in the RIMO experimental group then had an initial meeting with a linkage manager, were scheduled for treatment intake at a licensed detox facility, and were provided with transportation to the appointment. The linkage manager followed up multiple times a week with the individual and the treatment facility for the following four weeks. Individuals in the control group were given an informational brochure listing local treatment providers. Thirty days after study enrollment, the researchers conducted follow-up interviews with participants to measure opioid treatment received in the past thirty days (yes/no) and the number of treatment days, with a specific focus on MAT. The researchers also conducted a focus group with RIMO experimental group participants.
What did they find?
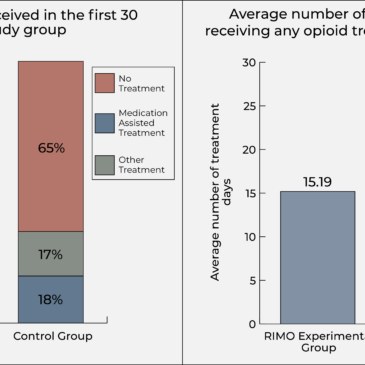
Participants in the RIMO experimental group were more likely to initiate any type of treatment compared to the control group (81% vs. 35%) and averaged more days in treatment over the 30-day study period (15.19 days vs. 3.41 days; see Figure). RIMO experimental group participants were more likely to engage in MAT specifically (81% vs. 18%) and were also more likely to be receiving MAT after 30 days (44% vs. 6%). Within seven days of initial contact with EMS personnel, 44% of the RIMO experimental group participants were admitted to MAT. Eighty-one percent were admitted to MAT within 28 days from initial contact. Focus groups revealed that participants felt favorably about their interactions with EMS personnel following naloxone administration and believed that this played a significant role in their engagement with treatment by linking them to the study team. In addition, participants felt positively about the assertive outreach, engagement, and persistent follow-up strategies employed by the linkage managers.

Figure. On the left: The percentage of study participants in the RIMO experimental group and the control group who engaged in each type of substance use treatment (no treatment, medication assisted treatment, other treatment) after their nonfatal overdose. On the right: The average number of treatment-days (out of 30) for participants of the RIMO experimental group and the control group. Adapted from Scott et al. (2020). Click image to enlarge.
Why do these findings matter?
Survivors of an opioid overdose are at high risk of repeated overdose. Although treatment for OUD — MAT in particular — reduces the risk of death following a nonfatal overdose, treatment engagement following an overdose is low. This study demonstrates that intervening with individuals immediately following an overdose may be beneficial for engaging this high-risk group into treatment, and that EMS personnel — who often respond to overdose events — can successfully initiate this linkage. Furthermore, this study demonstrates that combined assertive outreach, engagement, and follow-up strategies are effective in engaging high-risk individuals into any opioid treatment, and those individuals receive more treatment than their counterparts.
Every study has limitations. What are the limitations of this study?
This study had a small sample size, with only thirty-three participants. Given that the follow-up period was short, the long-term treatment retention and outcomes are unknown. In addition, this study took place within the City of Chicago, so the results may not be generalizable to other cities or areas.
For more information:
Are you worried that you or someone you know has an addiction? The SAMHSA National Helpline is a free treatment and information service available 24/7. For more details about addiction, visit our Addiction Resources page.
— Kira Landauer, MPH
What do you think? Please use the comment link below to provide feedback on this article.




David Wilson April 14, 2020
Since there are multiple possible MAT’s, it would be interesting to break those out.
My experience as a clinician has been that different medications seem to attract different populations, after taking into account the widely divergent availability of different medications in different areas.