In the United States alone, 47,600 people died due to prescription opioid overdoses in 2017, increasing by more than five-times between 1999 and 2017. During this same period, clinicians and researchers observed the therapeutic applications of medical marijuana for pain relief and as a potential substitute for opioid pain relievers. Opioid pain relievers have a wide range of side effects, including addiction and death, so providing safer alternatives to treat pain is important for medical professionals and their patients. This week, STASH reviews a study by David Powell and colleagues that examined how changes in medical marijuana laws affected deaths due to prescription opioids and heroin.
What was the research question?
Do medical marijuana laws reduce deaths from opioid and heroin overdoses? What is the effect of greater legal access to medical marijuana among qualified patients (i.e., through operational medical marijuana dispensaries)?
What did the researchers do?
The researchers analyzed state-level information about (1) medical marijuana laws and regulations, (2) medical marijuana dispensaries, and (3) and deaths from opioid-related overdoses. These records covered the period from 1999 to 2013.The authors studied how opioid-related deaths were related to medical marijuana laws/regulations and operating medical marijuana dispensaries (see Figure). Even though their study was cross-sectional, the authors drew conclusions about cause-and-effect by relying on advanced statistical techniques, including regression models that used a difference in differences approach and controlling for demographics, unemployment rates, alcohol tax rates, state prescription drug monitoring programs, and anti-“pill mill” laws.
What did they find?
The results showed that medical marijuana laws alone did not have a statistically significant effect on prescription opioid- or heroin-related deaths during the 1999-2013 period, controlling for the variables mentioned above. However, when the researchers added in a measure of whether states had operational medical marijuana dispensaries, the total effects of medical marijuana laws and operational dispensaries resulted in a 24% reduction in prescription opioid deaths and a 23% reduction in prescription opioid and heroin deaths combined.
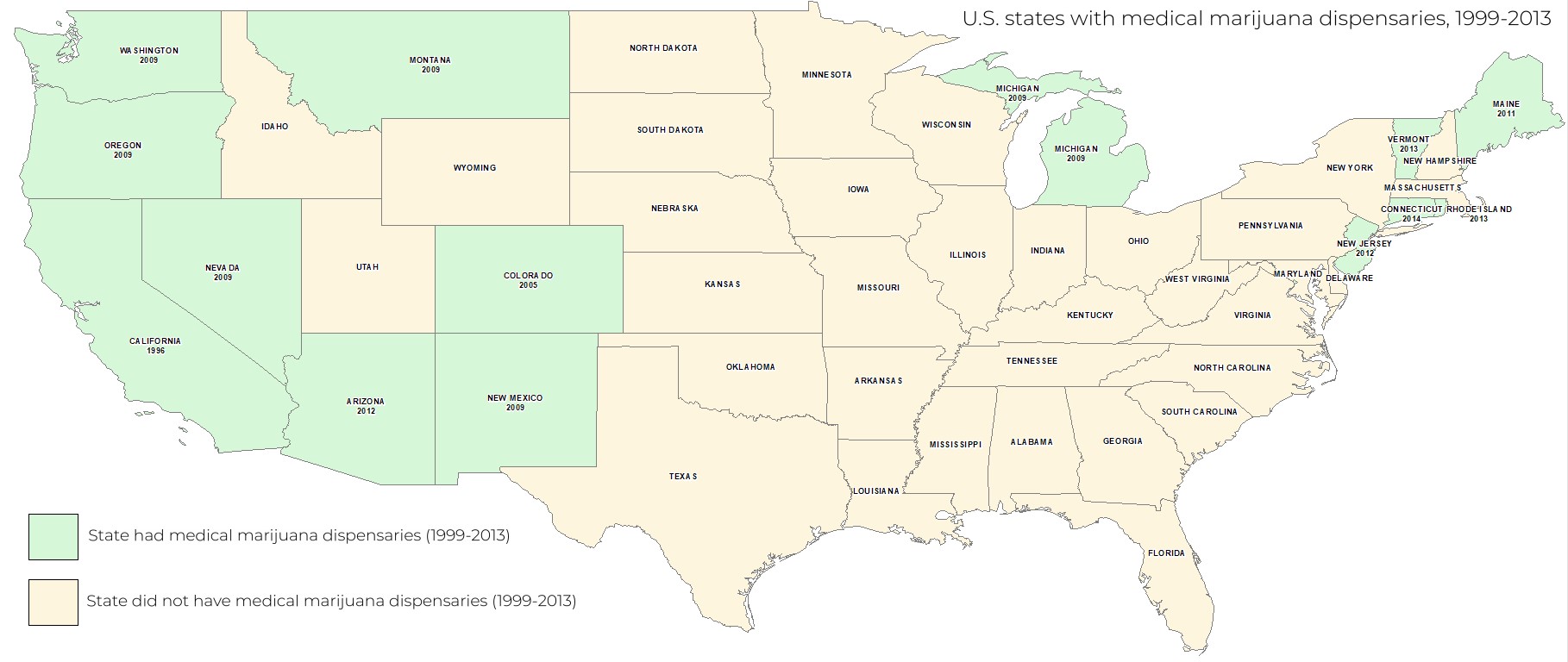
Figure. The year shown for states with medical marijuana dispensaries is the year that the first dispensary opened and began operating. Washington D.C. (not labeled on map) opened their first medical marijuana dispensary in 2013. Click image to enlarge.
Why do these findings matter?
These findings are important for medical professionals who work in pain management, as they suggest that medical marijuana can provide an alternative for people seeking to reduce pain without the many side effects associated with opioids. While marijuana does have side effects such as respiratory difficulties and psychosis in individuals predisposed to schizophrenia, it does not cause death by overdose, so its medical use for pain management could reduce harm due to opioids. The results can inform local, state and federal policymakers about one of the many approaches to combating the opioid epidemic, which requires a multifaceted solution including better addiction treatment, prescription tracking programs, and access to medications such as methadone and naloxone.
Every study has limitations. What are the limitations in this study?
Although the authors analyzed a large sample with fifteen years of data, the last year in their dataset is 2013, so the results do not capture the more recent effects of medical marijauana laws on opioid overdose deaths. Moreover, this study focused exclusively on medical marijuana laws, so it was unable to determine how more recent recreational marijuana legalization could affect opioid overdoses.
For more information:
Are you worried about your own or a loved one’s addiction or mental health issues? The National Helpline is a free treatment and information service that is available 24/7. For additional resources, please feel free to visit The BASIS Addiction Resources page.
— Eric R. Louderback, Ph.D.
What do you think? Please use the comment link below to provide feedback on this article.





Ken C. Winters July 9, 2019
Ugh!!! I am disappointed that the Powell study was highlighted in the absence of more rigorous publications on the issue of cannabis laws and opioid abuse. I point readers to these two articles. One is a viewpoint piece that includes a brief overview of the literature on this topic. The other examines state aggregate data over a longer period (1999-2017) than Powell’s study. These both cast doubt that pro-cannabis laws will aid the opioid crisis.
Humphreys, K., & Saitz, R. (2019). Should physicians recommend replacing opioids with cannabis?. JAMA, 321(7), 639-640.
Shover, C. L., Davis, C. S., Gordon, S. C., & Humphreys, K. (2019). Association between medical cannabis laws and opioid overdose mortality has reversed over time. Proceedings of the National Academy of Sciences, 116(26), 12624-12626.
Eric Louderback July 10, 2019
Thank you, Ken, for sharing these two additional studies that examined the medical marijuana law and opioid abuse relationship.
The articles you cited provide evidence suggesting that medical marijuana laws may not reduce opioid-related deaths over a longer period of time. You make great points in your comment and based on the two more recent studies, the scientific evidence suggests that pro-cannabis laws should not be recommended as a primary means of reducing opioid abuse and overdoses.
Given the importance of the opioid epidemic in the United States, we have included these two studies as potential articles for future BASIS posts.
Ken C. Winters July 17, 2019
Eric, thanks! And you and the group keep up the great work.