The DRAM previously reviewed a study showing that returning veterans with mild traumatic brain injuries (mTBIs) are at an elevated risk for developing alcohol and drug use disorders, compared to veterans with other kinds of injuries. This week, as part of our Special Series on Addiction among Military Personnel and Veterans, we explore how brain injuries and substance use impact the ability to function in daily life. More specifically, we review a study that examined how mTBI, PTSD, and long-term alcohol use relate to associative learning, an important aspect of brain functioning (McGlinchey et al., 2014).
Methods
- Participants were 81 veterans and active duty personnel who had been deployed to Operation Enduring Freedom (OEF) or Operation Iraqi Freedom (OIF).
- Researchers separated the participants into three groups.1
- Deployed Control (n=25): participants with no PTSD or mTBI diagnosis
- PTSD only (n=25): participants who met DSM-IV criteria for PTSD but had no mTBI
- Comorbid PTSD & mTBI (n=31): participants who both met DSM-IV criteria for PTSD and had an mTBI
- Participants in all three groups completed self-report measures of (1) lifetime alcohol consumption (frequency, amount, and duration) and (2) lifetime and past-year alcoholic behaviors.
- To study brain function, researchers used an eyeblink classical conditioning task that measures basic associative learning, cognitive function, and memory.
- In this task, the researchers repeatedly paired a tone (the conditioned stimulus) with a mild puff of air to the eye (the unconditioned stimulus). The air puff naturally produces an eyeblink. Over time, participants blink after the tone but before the air puff. In other words, they exhibit a conditioned response (CR), showing that the brain has associated the tone with the air puff.
- The researchers measured the percentage of test trials in which participants successfully produced a CR.
- In the delay conditioning trials, the tone and air puff overlapped in time.
- In the more complex trace conditioning trials, the tone occurred first, followed by a pause, followed by the air puff. Associating the tone and the air puff requires the formation of a memory “trace.”
- The researchers compared how the three groups differed in eyeblink conditioning performance.
- Researchers also explored how alcohol use, across all three groups, related to eyeblink conditioning performance.
Results
- All three groups— Deployed Controls, PTSD only, and Comorbid PTSD with mTBI—showed comparable eyeblink conditioning performance.
- However, across all three groups, alcohol use was associated with impaired delay and trace conditioning.
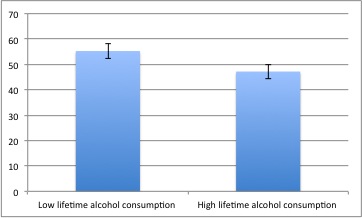
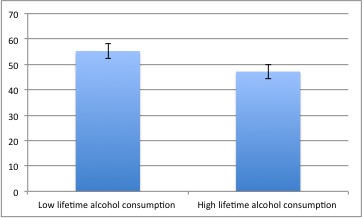
- In the Delay conditioning trials, lifetime alcohol consumption and lifetime alcoholic behaviors were negatively associated with the mean percent of CRs.
- In the Trace conditioning trials, lifetime alcohol consumption, as well as lifetime and past-year alcoholic behaviors, were negatively associated with the mean percent CRs.
Figure. Mean percentage CRs in trace conditioning trials, as a function of lifetime alcohol consumption. Participants were divided into 2 groups using a median split. Error bars represent standard errors. Click image to enlarge.
Limitations
- This study used a relatively small sample of participants, which limits the statistical power to detect group differences.
- A fourth group of participants who had mTBI only was too small to use for data analysis.
- The study results only demonstrate a negative association between alcohol abuse and associative learning; they do not prove that alcohol abuse is a direct cause of deficits in veterans’ associative learning abilities.
Conclusion
The negative impact of substance use disorders, including alcohol abuse, on public health is well documented. However, more research is needed to uncover the joint effects of post-war complications, including brain injury and substance use, on veterans’ re-entry into civilian life. These study results suggest that veterans can maintain intact basic associative learning and memory function after war, but that these abilities suffer with continued alcohol abuse. To better understand this phenomenon, researchers could use larger samples, study participants over a greater period of time, and examine how associative learning responds to substance use disorder treatment.
– Ingrid Maurice
What do you think? Please use the comment link below to provide feedback on this article.
Reference
McGlinchey, R., Fortier, C., Venne, J., Maksimovskiy, A., & Milberg, W. (2014). Effects of OEF/OIF-Related physical and emotional co-morbidities on associative learning: Concurrent delay and trace eyeblink classical conditioning. International Journal of Environmental Research Public Health; doi: 10.3390/ijerph110303046. http://www.mdpi.com/1660-4601/11/3/3046.
1 An additional group of participants who had only mTBI (N=7) only was too small data analysis.