I went to [an] emergency room one time and the lady came back after checking my record and barely talking to me; she said ‘well there is nothing we can do, we can’t help you here’ and she didn’t even get to talk to me; she was going by my records.
– An individual with a history of substance use disorder discusses an experience of stigma in a healthcare setting. From a study by Brondani, Alan, and Donnelly 2017.
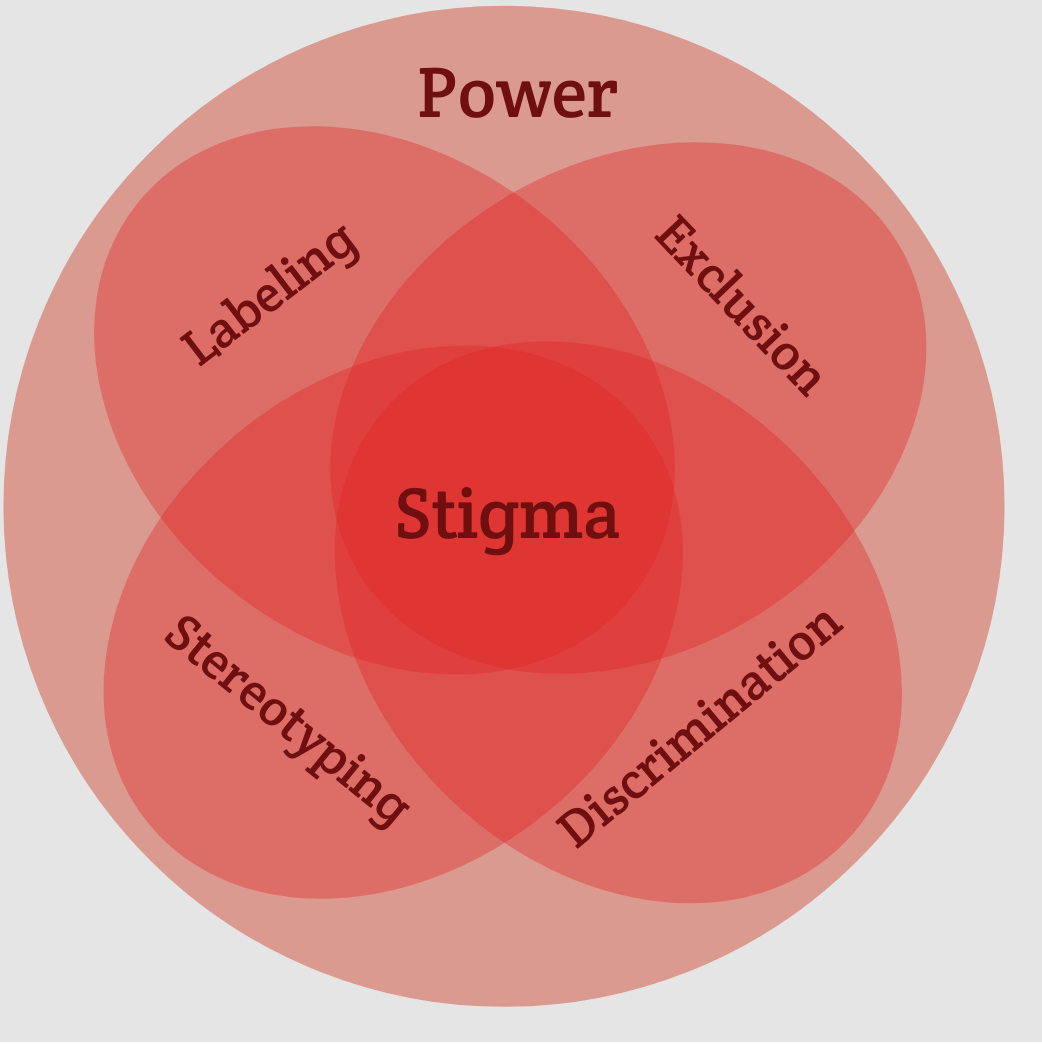
Figure. A conceptual model of stigma that locates discrimination, stereotyping, exclusion, and labeling within the context of power. Adapted from Brondani, Alan, and Donnelly 2017. Click the image to enlarge.
According to a nationally representative survey, 80% of people who have experienced alcohol use disorder and 75% of people who have experienced a drug use disorder have never sought treatment for their addiction. One of the reasons for these low rates of treatment seeking is stigma. It is no secret that addiction is a highly stigmatized disease. Historically, many have viewed addiction as a moral failing – a crime rather than a disease – and those who have experienced addiction have been branded with this stigma.
The effects of stigma go beyond hurt feelings. Stigma towards addiction has real, harmful consequences. Most of us understand stigma as what happens when a characteristic causes a person to be viewed as socially undesirable and leads to stereotyping, rejection, and discrimination. What we often fail to acknowledge, however, is that stigma is more than an interpersonal process – it is a systemic one. Stigma is deeply embedded with social, economic, and political power (see figure). Stigma can impact not only the willingness of a person experiencing addiction to seek treatment, but it can impact the funding and availability of public health initiatives meant to prevent and reduce addiction-related harm.
As we kick off this month’s Special Series on Stigma and Addiction, we will explore how aspects of stigma impact the experience of addiction. ASHES will discuss how patients’ perceptions of smoking-related stigma relate to their interactions with healthcare providers. STASH will review a study that examined associations between self-stigma, demographic characteristics, and injection risk behaviors among people who inject drugs in New York City. The WAGER will describe how people who are labeled as having Gambling Disorder face more stigma than those who are not. Finally, the DRAM will review a study examining how attitudes and beliefs towards seeking treatment for Alcohol Use Disorder changed over the course of a decade.
 We will supplement these reviews with two op-eds. The first is from a contributor who is dedicated to reducing addiction stigma. Michael Botticelli is the current Executive Director of the Grayken Center for Addiction at Boston Medical Center. He shares with us his insights from his time as the Director of National Drug Control Policy for the Obama administration and as a person in long-term recovery. The second is from Sydney Durand, the Massachusetts Director of Programs for The Phoenix. The Phoenix is a non-profit that provides a free sober active community for people in recovery. This spring, they partnered with the Red Sox to confront the stigma of addiction.
We will supplement these reviews with two op-eds. The first is from a contributor who is dedicated to reducing addiction stigma. Michael Botticelli is the current Executive Director of the Grayken Center for Addiction at Boston Medical Center. He shares with us his insights from his time as the Director of National Drug Control Policy for the Obama administration and as a person in long-term recovery. The second is from Sydney Durand, the Massachusetts Director of Programs for The Phoenix. The Phoenix is a non-profit that provides a free sober active community for people in recovery. This spring, they partnered with the Red Sox to confront the stigma of addiction.
We hope this Special Series provides an opportunity for learning and reflection for all our readers. We welcome thoughtful discussion in the comments below.
— Rhiannon Chou Wiley




Roger Howard May 8, 2019
Excellent to see this report.
You might want to look at substantial original research carried out in the United Kingdom for the UK Drug Policy Commission a few years ago about the pervasive nature of stigma:
https://www.ukdpc.org.uk/publication/getting-serious-about-stigma-problem-stigmatising-drug-users/
Rhiannon Wiley May 8, 2019
Thank you for sharing this report!