Veterans often face challenges when they return home from serving overseas. Unemployment is one such challenge. Some veterans might have trouble finding jobs because they are struggling with mental health problems, such as substance misuse, anxiety, post-traumatic stress disorder (PTSD), and depression. This week, STASH reviews a study of employment among vets with substance use disorders who either have, or do not have, co-occurring psychiatric and general medical conditions (Humensky et al., 2013). This review is part of our Special Series on Addiction among Military Personnel and Veterans.
Methods
- Participants were veterans who used the Veterans Administration (VA) for substance use disorder treatment between September 1, 2001 and February 10, 2010.
- Specifically, participants were 5,729 veterans (3% female; mean age = 49 years) who described their medical, employment/support, drug and alcohol use, legal, family/social, and psychiatric status at treatment intake and again 3-9 months later.1
- The authors used these interviews to code whether each participant had co-occurring anxiety, depression, suicidality, or general medical problems at intake.
- The authors also coded whether each participant had any earnings from employment and any days of paid work during the 30 days before the follow-up interview.
- The authors examined whether participants who had a co-occurring psychiatric or general medical problem at intake were less like to have any earnings and any days of paid work in the month before follow-up than participants without these conditions.2
Results
- When they began substance use disorder treatment, most veterans (72%) had no past-month earnings or days of paid work. At follow-up, 68% had no past-month earnings and 65% had no past-month days of paid work.
- As Figure 1 shows, veterans with co-occurring anxiety and with co-occurring general medical problems at intake were less likely to report any past-month earnings at follow-up than veterans without these conditions.
- For example, veterans with general medical conditions were less than half as likely to have past-month earnings. The same pattern emerged for having any days of paid work.
- Depression and suicidality were not associated with lower odds of having employment (Figure 1).
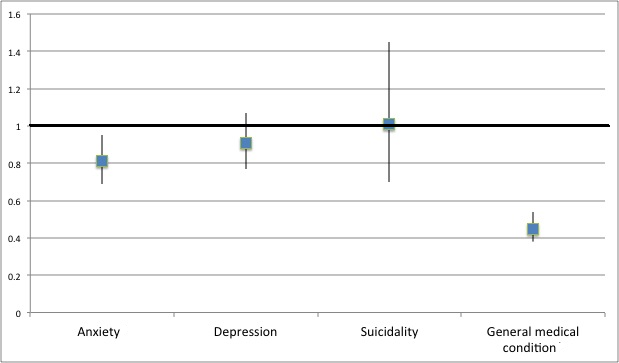
Figure. Odds ratios (blue boxes) and 95% confidence intervals (gray lines) for having any past-month earnings, depending on having each co-occurring psychiatric or general medical condition. When confidence intervals are completely below 1.0, the odds of having any earnings are lower among veterans with the corresponding co-occurring condition, compared to veterans without that condition. This is the case for anxiety and general medical condition. Adapted from Humensky et al. (2013). Click image to enlarge.
Limitations
- The authors did not categorize participants according to formal diagnoses of psychiatric and medical conditions. Instead, they relied on self-reports of problems that might have varied in their severity. More stringent criteria might have led to stronger results. Also, the authors did not have a specific measure of PTSD.
- The results of this study are not generalizable to nonveteran populations or to veterans who are not in substance use disorder treatment.
- The follow-up period (3-9 months) was fairly short.
Conclusion
Finding and keeping a job is an important part of daily life. The majority of veterans in substance use disorder treatment were unemployed both when they started treatment and at follow-up. Those who also experienced anxiety and general medical conditions were especially at risk for continued unemployment. Treatment providers should identify patients who are at higher risk for unemployment and try to connect them with supportive programs.
– Heather Gray
What do you think? Please use the comment link below to provide feedback on this article.
References
Humensky, J. L., Jordan, N., Stroupe, K. T., & Hynes, D. (2013). Employment Status of Veterans Receiving Substance Abuse Treatment From the U.S. Department of Veterans Affairs. Psychiatric Services, 64, 177-180.
McLellan, A.T., Luborsky, L., Cacciola, J., et al. (1985). Guide to the Addiction Severity Index: Background, Administration, and Field Testing Results. Washington, DC, US Government Printing Office.
________________
[1] This information came from the Addiction Severity Index, a semi-structured interview (McLellan et al., 1985).
[2] The authors used logistic random effects models including a random intercept by treatment site to account for clustering by treatment site. The authors controlled for demographic (gender, age, years of education, race, length of time from intake to follow-up, and number of ASI assessments completed during the study period).




