The dangers of second-hand smoke are well established. To protect nonsmokers from exposure to second-hand smoke and to encourage smokers to quit, states and municipalities have implemented a variety of policies prohibiting smoking in public buildings and open spaces, businesses, and even apartment buildings. This week’s ASHES reviews a meta-analysis of studies examining trends in cardiovascular and respiratory disease risk before and after implementation of smoke-free laws (Tan & Glantz, 2012).
Methods
- The research team used scientific databases, reference lists, and a network of tobacco control scientists to identify studies that examined the association between smoke-free laws and hospitalizations or deaths due to cardiovascular or respiratory disease.
- The meta-analysis included a total of 43 studies that had sufficient data to calculate the relative risk and confidence interval before and after implementation of a smoke-free law.
- The researchers categorized smoke-free laws based on comprehensiveness (i.e., applying only to workplaces versus workplaces, restaurants, and bars).
- The researchers categorized study outcomes into four groups: coronary events; other heart disease; cerebrovascular accidents; and respiratory disease.
- Across studies, the median window of observation before smoke-free legislation was 29.5 months, and the median window of observation after smoke-free legislation was 24
months. - The researchers performed a random-effects meta-analysis for each outcome group stratified by comprehensiveness of laws.
Results
- Researchers found that implementation of a smoke-free law was associated with lower rates of hospital admission or death for all four outcome groups
- Coronary events (Relative Risk [RR] = 0.85; 95% Confidence Interval (CI) 0.82–0.88)
- Other heart disease (RR = 0.61; 95% CI [0.44–0.85])
- Cerebrovascular accidents (RR = 0.84; 95% CI [0.75– 0.94])
- Respiratory disease (RR = 0.76; 95% CI [0.68–0.85])
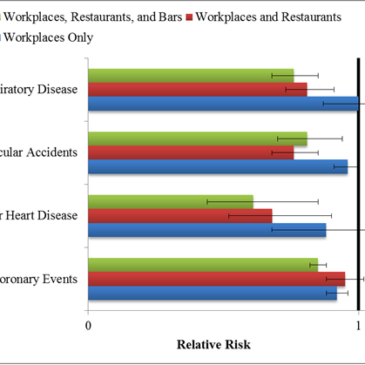
- As Figure 1 shows, more comprehensives laws produced greater reductions in risk for related health outcomes.
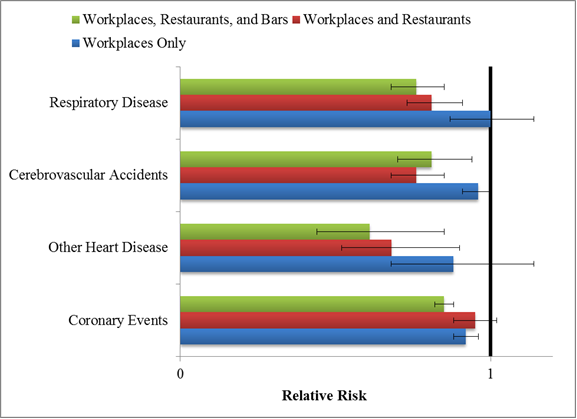
Figure. Relative risk of hospital admissions for disease categories after implementation of smoke-free law compared with before implementation. (Adapted from Tan and Glantz, 2012). Click image to enlarge.
Note. RRs less than 1 indicate less population risk after implementation of a smoke-free law; across outcome groups, law comprehensiveness significantly predicted risk, p < .002.
Limitations
- Few of the included studies measured smoking status or exposure among individuals, making it difficult to understand the underlying mechanism that led to reductions in
Relative Risk for the related diseases.- Potential mechanisms include smoking cessation, changes in social norms, reductions in exposure to secondhand smoke, and some combination of these.
- Publication bias—the tendency for studies with null effects not to be published— is a concern with all meta-analyses and might bias the results away from the null.
- Only a randomized, controlled trial can truly establish causation. The studies used in this meta-analysis used interrupted time series observational studies. These results should be interpreted in light of other pieces of evidence (e.g., known biological pathways by which tobacco smoke exposure causes disease) that, together, suggest a causal link between smoke-free laws and reduced risk of disease.
Conclusions
This study supports the findings of previous research and further clarifies the relationship between smoke free laws and related health outcomes. Specifically, in addition to associations between smoke-free laws and lower risk of related health outcomes, researchers also found a dose-response relationship between the comprehensiveness of the law and that risk. Interpreted in light of other pieces of evidence (e.g., known biological pathways by which tobacco smoke exposure causes disease) these findings suggest a causal link between smoke-free laws and reduced risk of disease and provide a strong evidence-base for policy decisions.
-John Kleschinsky
Refererences
Tan, C. E., & Glantz, S. A. (2012). Association between smoke-free legislation and hospitalizations for cardiac, cerebrovascular, and respiratory diseases. Circulation, 126(18), 2177-2183.