Both physiological and behavioral evidence suggest that we might be able to view excessive eating as an expression of addiction. Previous studies suggest that food and alcohol consumption might compete for the same biological pathways (Kleiner et al., 2004). If so, one would expect that engagement in one of these behaviors might lessen engagement in the other. This week’s DRAM reviews a paper that examines the relationship between excessive food and alcohol consumption (Gearhardt & Corbin, 2009).
Method
- Participants and procedure
- Investigators interviewed more than thirty five thousand participants as a part of the National Epidemiologic Survey on Alcohol and Related Conditions (NESARC: Grant, 1997), a nationally representative general population survey.
- Measures of interest
- Investigators assessed two measures of alcohol consumption: frequency of use and blood alcohol level. Typical blood alcohol level was estimated based on the reported frequency of use (number of drinking days in the past year) and quantity of drinking (drinks per drinking day), sex and weight.
- In addition, the researchers collected data on family history of alcohol problems and BMI (Body Mass Index) for each participant. See Figure 1 for weight categorization.
Results
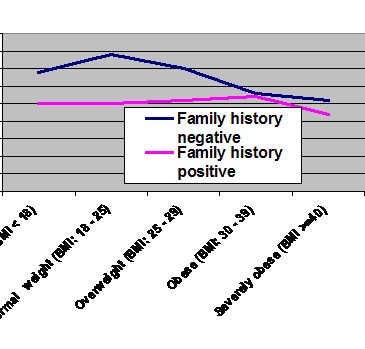
- Obese participants consumed alcohol significantly less frequently than normal weight and overweight participants (F (4, 37502) = 34.47, p < .001).
- Family history of alcohol problems predicted frequency of alcohol consumption for nonobese participants (F (1, 28544) = 97.26, p < .001), but not for obese participants (F (1, 8971) = 2.577, p = .28) (see Figure).
- Family history of alcohol problems predicted blood alcohol level both for obese and nonobese participants; however its effect for nonobese participants was much higher (2= .012 vs. 2= .001)
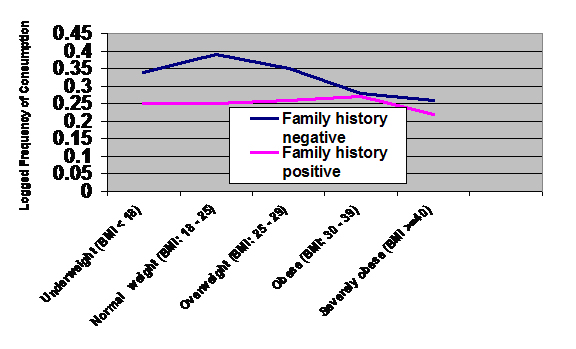
Figure. The effect of weight category and family history of alcohol problems on the frequency of alcohol use. Click image to enlarge.
Limitations
- Self-reported results
- No direct test of excessive eating. Obesity suggests but does not require excessive eating behavior.
- The findings suggest food and alcohol consumption might share the same biological pathway; however, this mechanism was not tested directly.
Conclusion
The authors conclude that the results provide additional support for the hypothesis that alcohol consumption and excessive eating share the same neurobiological pathways and both might be categorized as expressions of addiction, a conclusion consistent with the Syndrome Model of Addiction (Shaffer et al., 2004). However, the inverse relation between obesity and alcohol consumption is contradictory to other findings that demonstrate the multimorbidity of different expressions of addiction (McKee et al., 2009; also see DRAM 5(5)). Future research needs to investigate both the mechanisms through which multiple expressions of addiction arise and the course of those expressions within individuals who develop more than one expression.
What do you think? Please use the comment link below to provide feedback on this article.
References
Gearhardt, A. N., & Corbin, W. R. (2009). Body mass index and alcohol consumption: Family history of alcoholism as a moderator. Psychology of Addictive Behaviors, 23(2), 216-225.
Grant, B. F. (1997). Prevalence and correlates of drug use and DSM-IV alcohol dependence in the United States: Results of the National Longitudinal Alcohol Epidemiologic Survey Journal of Studies on Alcohol 58, 464-473.
Kleiner, K. D., Gold, M. S., Frost-Pineda, K., Perri, M. G., Jacobs, W. S., & Lenz-Brunsman, B. (2004). Body Mass Index and Alcohol Use. Journal of Addictive Diseases, 23(3), 105-118.
McKee, S. A., Harrison, E. L., O’Malley, S. S., Krishnan-Sarin, S., Shi, J., Tetrault, J. M., et al. (2009). Varenicline reduces alcohol self-administration in heavy-drinking smokers. Biological Psychiatry (In Press).
Shaffer, H. J., LaPlante, D. A., LaBrie, R. A., Kidman, R. C., Donato, A. N., & Stanton, M. V. (2004). Toward a syndrome model of addiction: Multiple expressions, common etiology. Harvard Review of Psychiatry, 12, 367-374.