Chemical treatments abound in today’s society for almost any condition or perceived deficit. Whether it involves taking diet pills to lose weight, anti-depressants to fight the blues, or Ginkgo to improve memory, we often look to medication (of greater or lesser scientific merit) for a solution to our problems. However frivolously they have been used elsewhere, pharmacological treatments have had significant impact on the chemical addictions. Recovering heroin users have been taking methadone since the 1970’s and people who are trying to quit smoking can take Zyban to reduce cravings and withdrawal symptoms. But what about treatment for pathological gambling (PG), a non-substance-related addiction? If PG was as responsive to chemical treatments as nicotine dependence and heroin dependence appear to be, this evidence would support the idea that behavioral addictions are analogous to substance-related addictions. While pharmacological treatment is new territory for PG patients, several studies have already been conducted examining the efficacy of drug therapy. A recent preliminary study conducted by Black (2004) tested the efficacy of the psychostimulant bupropion (Wellbutrin) for the treatment of PG.
As a psychostimulant, bupropion is used primarily to treat attention deficit hyperactivity disorder (ADHD). Specker and colleagues (1995) found a high comorbidity between PG and ADHD, leading them to believe the ADHD symptoms of impulsivity and attention deficit might make individuals more vulnerable to substance abuse and PG. This suspected link influenced Black’s choice of bupropion as a possible treatment for PG.
Black used advertisements to recruit ten subjects (six women and four men) who had scores of >=5 on the South Oaks Gambling Screen (SOGS) and met DSM-IV criteria for PG with symptoms lasting for at least one year. A diagnosis of ADHD was not required for inclusion – only one subject met criteria for ADHD. Subjects who had current diagnoses of schizophrenia, anxiety disorders, bipolar disorders, eating disorders, seizure disorders, or substance use disorders were excluded from participating in the study. At baseline and each week during the eight-week study, subjects completed: a) the Yale- Brown Obsessive-Compulsive Scale Pathological Gambling Version (YBOCS-PG) to determine the severity of PG; b) the Attention Deficit Hyperactivity Disorder (ADHD) checklist to measure symptoms of ADHD; c) the Hamilton Rating Scale for Depression (HRDS); d) the Clinical Global Impression Inventory (CGI) to measure gambling symptom improvement; and e) the Sheehan Disability Scale (SDS) to assess disability in their family, social, and work lives. Black started subjects with a dosage of 100 mg daily of slow release bupropion, increased the daily dose by 100 mg each week for three weeks, and then had subjects maintain a steady dosage for 5 more weeks.
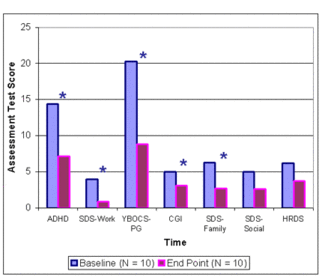
Figure 1: Changes in Assessment Scores during 8-week Bupropion Treatment
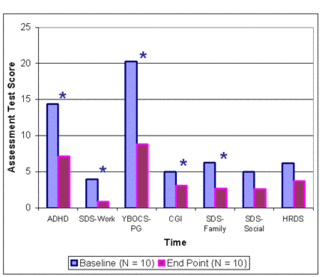
* = significant difference (p < .01) on paired t-test, baseline to endpoint.
Note: Assessments are ordered according to effect size. Three subjects did not complete the week 6 and week 8 visits. Their week 4 scores were counted as their end point scores.
As shown in Figure 1, between baseline and end point (i.e., week 8 for seven subjects and week 4 for three subjects), subjects’ PG severity (according to both the YBOCS and the CGI), ADHD scores, and work and family life disabilities significantly decreased. Seventy percent of the sample reported gambling symptoms as “very much improved” or “much improved”.
Subjects showed significant improvement on five of seven assessments from baseline to end point; however, this study has several limitations. It is a preliminary study of a small number of subjects that lacks a placebo control condition. The lack of a control group makes it impossible to rule out a placebo effect as the primary contributor to the decreases.
Despite its limitations, this preliminary study is the first to explore the effectiveness of a psychostimulant in treating PG; the results encourage more rigorous research on pharmacological therapies for the treatment of PG. There have been studies on other medications for the treatment of PG that also showed efficacy. Kim et al. (2001) conducted a double-blind placebo-controlled study of 45 patients testing the efficacy of naltrexone (commonly used to treat alcoholism or opiod dependence) for the treatment of PG and found that 75% of the subjects on naltrexone compared to 24% of the placebo subjects had improved CGI scores. Another double-blind study by Hollander et al. (2000) found that the selective serotonin reuptake inhibitor (SSRI) fluvoxamine (most commonly used to treat obsessive compulsive disorder) was an effective treatment for PG (see WAGER 4(1) for a review of Hollander’s preliminary study).
The results of these studies cited above suggest that pathological gamblers respond to different types of pharmacological treatment because pathological gamblers as a group include people with a variety of underlying antecedents or correlates of PG (e.g., depression, substance abuse, or ADHD). The study outcomes also contribute to the evidence that pharmacological treatments can be applied successfully to behavioral as well as chemical addictions. These findings have implications for the way we understand addiction. Both chemical and behavioral treatments appear to have similar efficacy in treating chemical and behavioral addictions, and both behavioral and chemical addictions share similar behavioral and neurochemical antecedents and consequences. Therefore, the distinction between the chemical and behavioral addictions and their treatment might be a less important distinction than variations in other aspects of addiction (e.g., comorbid conditions).
Comments on this article can be addressed to Alexa Rubenstein or Sarah Nelson.
References
Black, D. W. (2004). An open-label trial of bupropion in the treatment of pathologic gambling. Journal of Clinical Psychopharmacology, 24(1), 108-110.
Hollander, E., DeCaria, C. M., Finkell, J. N., Begaz, T., Wong, C. M., & Cartwright, C. (2000). A randomized double-blind fluvoxamine/placebo crossover trial in pathologic gambling. Biological Psychiatry, 47(9), 813-817.
Kim, S. W., Grant, J. E., Adson, D. E., & Shin, Y. C. (2001). Double-blind naltrexone and placebo comparison study in the treatment of pathological gambling. Biological Psychiatry, 49, 914-921.
Specker, S. M., Carlson, G. A., Christenson, G. A., & Marcotte, M. (1995). Impulse control disorders and attention deficit disorder in pathological gamblers. Annals of Clinical Psychiatry, 7(4), 175-179.