Gambling has joined drinking, drugs, and breaking curfew as one of those activities adults believe adolescents do too much. Estimates of adolescent gambling problems support this view – adolescents consistently demonstrate higher prevalence rates of disordered gambling than adults (Shaffer & Hall, 2001). Yet, despite these elevated rates, adolescents rarely seek treatment (Gupta & Derevensky, 2000). This week’s WAGER reviews an article by Hardoon, Deverensky, and Gupta (2003) that attempts to explain this discrepancy and raises questions about the role of perception and awareness in the measurement of disorders.
Hardoon and her colleagues (2003) recruited 980 students (M = 18.6 years old, SD = 1.69) from junior colleges in Montreal to complete four different assessments of disordered gambling (administered in a randomized order). The screens included the adolescent version of the South Oaks Gambling Screen (SOGS-RA) (Lesieur & Blume, 1987; Winters, Stinchfield, & Fulkerson, 1993), an adolescent version of the DSM-IV criteria for pathological gambling (DSMIV-J) (Fisher, 1992), the GA 20 Questions screen, and the Gambling Activities Questionnaire. The first three arrive at diagnoses of disordered gambling (“problem” and “probable pathological”) by comparing endorsed symptoms against established cutpoints for levels of gambling disorders, whereas the Gambling Activities Questionnaire asks respondents to rate themselves on a 7 point Likert scale as social, problem, or pathological gamblers.
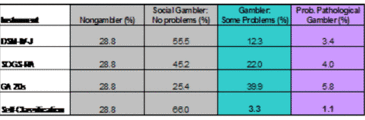
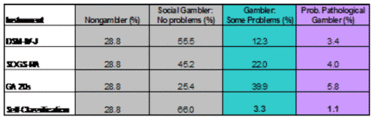
Table 1. Classification of Problem and Probable Pathological Gamblers by Screens and Self-Rating (Hardoon et al., 2003).
As Table 1 shows, only 4.4% of participants rated themselves as having any gambling related-problems (i.e., some problems 3.3% + pathological gambler 1.1%). The most conservative screen, the DSM-IV-J, identified almost four times more disordered gamblers than did self-report, .2(1) = 72.4, p < .001. The SOGS, one of the most commonly used assessments in the field, identified six times more disordered gamblers than self-report, .2(1) = 182.1, p < .001. Of the participants classified by the screens as probable pathological gamblers (3.4% to 5.8% of the sample), only 8.9% to 18.8% rated themselves as pathological gamblers and 37.5% to 58.9% rated themselves as having no gambling problems. Conversely, four participants rated themselves as pathological but did not meet diagnostic criteria.
Hardoon et al. interpret the discrepancy between self-ratings and the range of screens as proof that adolescents do not perceive or are not willing to identify their gambling behavior as problematic. However, the experimental design places some limitations on this interpretation. First, Hardoon et al. tailor their interpretation toward adolescents even though there is no evidence that their results do not also apply to adults. In fact, they drew their sample from a post-high school junior college population; thus, the findings might not be representative of all adolescents or exclusively applicable to adolescents who fail to seek treatment for gambling disorders. Second, Hardoon et al. use the DSM-IV-J’s stringency as grounds for dismissing the idea that all screens might over-identify gambling problems. However, the fact that one screen is more conservative than others does not itself validate that screen as more accurate. So long as the field has no gold standard of diagnosis, screening accuracy, in the strictest sense, cannot be determined.
Hardoon et al.’s results suggest that many adolescents do not report and, arguably, do not perceive gambling problems where screens purport that they exist. These findings provide a plausible explanation for adolescents’ failure to seek treatment and suggest that, as Hardoon et al. advise, campaigns to increase self-awareness of gambling problems might be a promising intervention strategy.
More generally, this study leads to two possible conclusions: (1) gambling screens over-classify individuals as disordered gamblers, or (2) disordered gamblers do not report and potentially do not perceive their “symptoms” as problematic. The former implicitly holds self-assessment as the standard by which screens ought to be measured and the latter excludes individuals’ awareness of their problem from the assessment of a disorder. Although it is unlikely that self-perception can be used as the measure of diagnostic validity, it remains unclear what role self-perception and subjective experience do play in assessment, diagnosis, and treatment. Is a problem a problem before the “disordered” individual identifies it as such? When the self-reported impact of disorder symptoms on an individual’s life is used as a criterion for diagnosis, research finds much lower rates of mental disorders than traditional screens (Narrow, Rae, Robins, & Regier, 2002). Can a problem be treated without such self-identification?
Stages-of -change treatment models (see Prochaska & DiClemente, 1982) consider patients’ self-perception of their problem as a crucial factor in guiding treatment. Studying the role of self-perception in the development, identification, treatment, and recovery from gambling and other mental health disorders might be a crucial step toward understanding the etiology and course of gambling and other disorders.
Comments on this article can be addressed to Sarah Nelson.
References
Fisher, S. E. (1992). Measuring pathological gambling in children: The case of fruit machines in the U.K. Journal of Gambling Studies, 8(3), 263-285.
Gupta, R., & Derevensky, J. L. (2000). Adolescents with gambling problems: From research to treatment. Journal of Gambling Studies, 16(2-3), 315-342.
Hardoon, K., Derevensky, J. L., & Gupta, R. (2003). Empirical measures vs. perceived gambling severity among youth: Why adolescent problem gamblers fail to seek treatment. Addictive Behaviors, 28, 933–946.
Lesieur, H. R., & Blume, S. B. (1987). The South Oaks Gambling Screen (SOGS): A new instrument for the identification of pathological gamblers. American Journal of Psychiatry, 144(9), 1184-1188.
Narrow, W. E., Rae, D. S., Robins, L. N., & Regier, D. (2002). Revised prevalence estimates of mental disorders in the United States: Using a clinical significance criterion to reconcile 2 surveys’ estimates. Archives of General Psychiatry, 59, 115-123.
Prochaska, J. O., & DiClemente, C. (1982). Transtheoretical therapy toward a more integrative model of change. Psychotherapy: Theory, Research and Practice, 19(3), 276-287.
Shaffer, H. J., & Hall, M. N. (2001). Updating and refining prevalence estimates of disordered gambling behaviour in the United States and Canada. Canadian Journal of Public Health, 92(3), 168-172.
Winters, K. C., Stinchfield, R. D., & Fulkerson, J. (1993). Toward the development of an adolescent gambling problem severity scale. Journal of Gambling Studies, 9(1), 63-84.