Conventional wisdom and clinical experience suggest that alcohol dependence (AD) is highly comorbid with pathological gambling (PG). Unfortunately, the evidence from studies is mixed; disparities abound for prevalence estimates of both PG and AD and few studies have included both disorders. In this week’s WAGER, we report the results of several prevalence studies including a recent national study (Welte et al., 2001) designed to measure the prevalence of comorbid PG and AD (Table 1). As will be discussed below, we suggest that methodological differences and limitations contribute to variations in reported prevalence rates. It is also suggested that meta-analysis might be a beneficial technique for attenuating the influence of these factors on our assessments of the frequency of PG and AD.
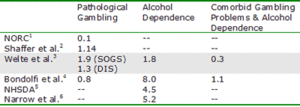
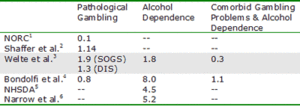
Table 1: Prevalence estimates for past-year pathological gambling, past-year alcohol dependence and comorbidity for alcohol and gambling pathology as reported in various studies, in percents
1. The National Opinion Research Center reported level 3 scores on the NORC DSM-IV Screen for Gambling Problems (NODS), which is approximately equal to PG (Gerstein et al., 1999) For more information, please refer to WAGER 6(30).
2. The Shaffer, Hall & Vander Bilt data is based on a meta-analysis (Shaffer, Hall & Vander Bilt, 1997)
3. The South Oaks Gambling Screen (SOGS-R) and the DIS-IV were used to assess pathological gambling; the DIS for DSM-IV was used to measure alcohol dependence (Welte et al., 2001)
4. National estimates for Switzerland were assessed using a revised version of the SOGS for gambling and the CAGE questionnaire for alcoholism (Bondolfi et al., 2000). For more information, please refer to WAGER 5(26).
5. Based on combined data from the 1997 and 1998 National Household Survey on Drugs and Alcohol (NHSDA, 2000)
6. Narrow et al. applied clinical significance criterion to the data from the National Institute of Mental Health Epidemiological Catchments Area Program (ECA) and the National Comorbidity Survey (NCS) (Narrow et al., 2002)
The Welte study, the Bondolfi study and the meta-analysis preformed by Shaffer et al. support a prevalence estimate for PG somewhere around 1-2%. However, the NORC study generated a PG prevalence estimate (0.1%) that falls far below this range. When we examine the prevalence of AD, we again find most estimates fall with in a general range (4.5% to 8.0%); yet the prevalence estimate from the Welte study is considerably lower at only 1.8%. As AD is one component of the comorbidity analysis, one would expect the comorbidity prevalence estimate to be low as well. Indeed, they report a lower prevalence of comorbid gambling problems and alcohol dependence than Bondolfi et al. (0.3% v. 1.1%). It is important to note, however, that Welte et al. calculated comorbidity prevalence estimates for AD and pathological gambling; Bondolfi et al. generated comorbidity estimates using a combined problem and pathological gambling group.
Since there is no “gold” standard for what constitutes pathological gambling or alcohol dependence, researchers employ different definitions and survey instruments to measure these disorders. This makes it difficult to verify the accuracy of any one estimate. Most instruments consist of a list of questions about the person’s behavior relating to gambling or alcohol and how it affects his or her personal life. Pathology is typically determined by the number of questions answered in the affirmative. Subtle differences in the questions asked and the number of affirmative answers the researchers use to classify them can alter the prevalence estimates. For example, Narrow et al. used clinical significance (treatment-seeking) to define alcohol dependence; therefore their rate represents a conservative estimate. Yet, the Welte et al. 1.3% prevalence estimate for alcohol dependence is still far below the 5.2% prevalence estimate generated by the stricter criteria of the Narrow study.
In addition to measurement differences, prevalence estimates also can be affected by sample methodology and sample size. For example, Welte et al. interviewed 2,638 adults, and found only nine respondents that reported comorbid AD and PG. Although 2,638 might seem like a satisfactory number, it represents merely one in 100,000 U.S. adults (U.S. Census Bureau, 2002). By contrast, the NHSDA and the ECA study (used by Narrow et al.) each interviewed about 1 in 10,000 U.S. adults; the Bondolfi study had the largest sampling fraction of all the studies, interviewing approximately 1 of every 2,000 Swiss adults. Small sample size might bias estimates.
When extensive cost prohibits the use of an adequately large sample size, an alternative strategy that can be employed to measure prevalence is meta-analysis (Shaffer et al., 1997). A metaanalysis is the statistical combination of data from a large collection of independent studies. Meta-analytic techniques are beneficial because the meaningfulness and value of evidence accrues; the potential bias in a single study can be offset by combining several studies. This suggests that meta-analytically combining well-done regional prevalence studies might provide better national estimates than small sample national studies.
A national prevalence estimate of comorbidity for gambling and alcohol pathology could be be applied to many areas from prevention efforts to public policy. However, as this WAGER has shown, we have not reached a consensus with regard to the prevalence estimates of the individual disorders, let alone that of comorbidity. We suggest careful and critical reading before drawing on the results of any study—meta-analytic or otherwise—because despite a “…review process to minimize errors, it is likely that in any project of this size there are over-looked details, and surely judgment calls for specific studies on which reasonable colleagues would disagree” (Miller et al., p. 31).
Comments on this article can be addressed to Rachel Kidman.
References
Bondolfi, G., Osiek C., Ferrero F. (2000). Prevalence estimates of pathological gambling in Switzerland. Acta Psychireica Scandinavica, 101: 473-475.
Gerstein, D., Murphy, S., Toce, M., Hoffmann, J., Palmer, A., Johnson, R., Larison, C., Chuchro, L., Bard, A., Engelman, L., Hill, M.A., Buie, T., Volberg, R., Harwood, H., Tucker, A., Christiansen, E., Cummings, W., & Sinclair, S. (1999). Gambling Impact and Behavior Study: Report to the National Gambling Impact Study Commission. Chicago: National Opinion Research Center.
Miller, W.R., Brown, J.M., Simpson, T.L., Handmaker, N.S., Bein, T.H., Luckie, L.F., Montgomery, H.A., Hester, R.K., & Tonigan, J.S. (1995). What works? A methodological analysis of the alcohol treatment outcome literature. In R.K. Hester & W.R. Miller (Eds.), Handbook of alcoholism treatment approaches: Effective alternatives (2nd ed., pp. 12-44). Boston: Allyn and Bacon.
Narrow, W.E., Rae, D.A., Robins, L.N., & Regier, D.A. (2002). Revised prevalence estimates of metal disorders in the United States: Using a clinical significance criterion to reconcile 2 surveys’ estimates. Archives of General Psychiatry, 59: 115-123.
Office of Applied Studies (1999). Summary of Findings from the 1998 National Household Survey on Drug Abuse. Rockville, MD, Department of Health and Human Services, Substance Abuse and Mental Health Services Administration.
Shaffer, H., Hall, M. & Vander Bilt, J. (1997). Estimating the prevalence of disordered gambling behavior in the United States and Canada: A meta-analysis. American Journal of Public Health.
U.S. Census Bureau, Population Division. Retrieved May 8, 2002 from the World Wide Web: http://www.census.gov.
Welte, J., Barnes, G., Weiczorek, W., Tidwell, M, & Parker, J (2001). Alcohol and gambling pathology among U.S. adults: prevalence, demographic patters and comorbidity. Journal of Studies on Alcohol, 62: 706-712.