STASH, Vol. 12(6) – When it comes to methadone maintenance treatment, one size does not fit all
Did you know that methadone maintenance treatment (MMT), is one of the most effective treatments for opioid use disorders, especially when patients stay in treatment for at least 12 months? In fact, stopping MMT prematurely risks negative outcomes, including death. As a result, a group of researchers recently studied which patients are most at risk for stopping MMT too soon. Today, as part of our Special Series on Opioid Dependence and Recovery, we review their study.
What is the research question?
Which factors predict stopping methadone maintenance treatment too early?
What did the researchers do?
Steven Proctor and his colleagues gathered patient record data from a large substance use treatment program in the United States. They used data from 1,644 MMT patients. The modal patient was male, between 18-74 years old, White, and unemployed. The researchers used logistic regression to determine what characteristics predicted being discharged from treatment before 6 months and before 12 months. The most common reason for discharge was leaving against medical advice.
What did they find?
Almost 50% of the patients were still in treatment 6 months after starting, and about 20% were still in treatment at 12 months. Some predictors warned of discharge just a few months after starting treatment. Specifically, being Hispanic, unemployed, and single, and using cocaine at intake all increased the risk for being discharged before 6 months. Other predictors warned of discharge later, but still prematurely. Male gender, being younger than 35, paying for treatment out-of-pocket, cocaine use at intake, and opioid use at 6 months all predicted discharge before the 12 months. In fact, patients who used cocaine at intake were nearly 4 times more likely to be discharged at 12 months (see Figure 1). Being on a relatively low dose of methadone also increased the risk for premature discharge.
Why do these findings matter?
Opioid dependence is complex and influenced by many factors, so treatment should not be one-size-fits-all. Armed with these results, treatment providers can devote specialized resources to patients who are most at risk for early discharge from MMT. For example, providers could connect unemployed patients with job skills programs, so they will have fewer barriers to staying in treatment for the long term. Similarly, patients from ethnic minority groups might benefit from culturally adapted treatments, unmarried patients might benefit from programs that strengthen their social networks, and patients using cocaine might benefit from psychosocial approaches (e.g., cognitive-behavioral therapy, contingency management) embedded within their MMT.
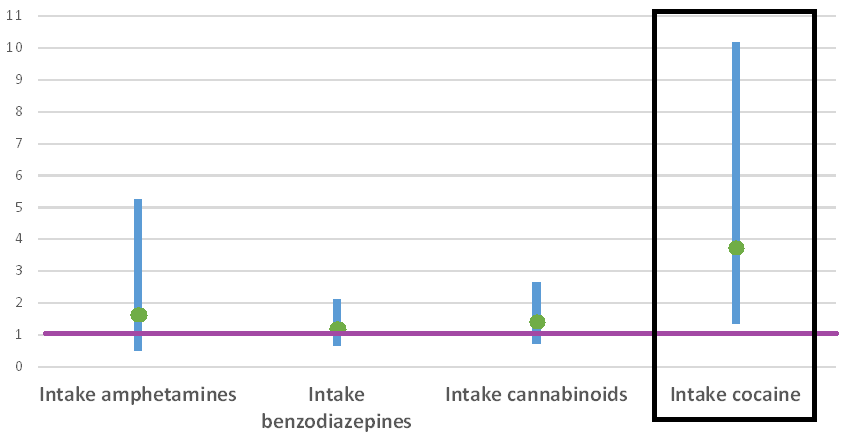
Figure. Substance use predictors showing increased risk of being discharged from MMT before 12 months. The green circles represent odds ratios and the blue lines represent 95% confidence intervals. Odds ratios greater than 1 indicate increased risk for premature discharge. The effect is only statistically significant for cocaine use at intake. Click image to enlarge.
Every study has limitations. What about this one?
Although the researchers have found that certain behaviors, like using cocaine at the start of MMT, predict increased risk for premature discharge, they cannot be certain that these behaviors cause increased risk. For example, using cocaine at intake could be a proxy for other characteristics that cause premature discharge. Still, these indicators help pinpoint patients who might need additional support to stay in treatment.
For more information:
The National Institute on Drug Abuse provides more information about methadone maintenance therapy and other treatments for opioid dependence here. You can find U.S. providers who treat substance use disorders here.
— Heather Gray
What do you think? Please use the comment link below to provide feedback on this article.