STASH Vol. 4(4) – You cannot always get what you need: Racial/ethnic disparities of opioid analgesic prescribing in U.S. emergency departments
Pain lasting more than 24 hours affects over one quarter of Americans each year (National Center for Health Statistics, 2006) and costs approximately $100 billion in lost productivity, lost income, and health care costs (Stewart, Ricci, Chee, Morganstein, & Lipton, 2003). Previous research examining U.S. emergency department visits from 1997 to 1999 found racial/ethnic disparities in the prescribing of opioid analgesics for back pain and migraines (Tamayo-Sarver, Hinze, Cydulka, & Baker, 2003). During 2001, the Joint Commission on Accreditation of Healthcare Organizations (JCAHO) established standards of care for the management of pain (Chapman, 2000). This week’s STASH examines the rates of opioid prescribing before and after the implementation of JCAHO standards of care among visits to the emergency room for the treatment of pain in the U.S. (Pletcher, Kertesz, Kohn, & Gonzales, 2008).
Pletcher, Kertesz, Kohn, & Gonzales (2008) analyzed prescriptions related to approximately 375,000 emergency room visits over the course of 13 years (1993-2005). The authors utilized data from the National Hospital Ambulatory Medical Care Survey (NHAMCS), a publicly available data set that uses a 4-stage probability sample design each year at randomly selected hospitals, excluding federal, military, and Veterans Administration hospitals, across the U.S. NHAMCS data include patients’ demographics, reasons for visit, diagnoses, and treatment. The authors analyzed NHAMCS data for patients with pain-related symptoms (e.g. pain, ache, soreness) and conducted logistic regression analyses to estimate the association between a doctor prescribing an opioid and race/ethnicity across time.
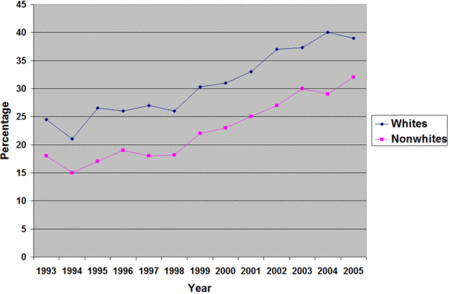
Figure. Percentage of emergency department pain-related visits for which a doctor prescribed an opioid analgesic by race/ethnicity and survey year (adapted from Pletcher, Kertesz, Kohn, & Gonzales, 2008). Click image to enlarge.
During the study period, the percentage of pain related visits that resulted in an opioid prescription increased from 23% (95% CI, 21%-24%) during 1993 to 37% (95% CI, 34%-39%) during 2005 (significant linear trend, p<.001). As figure 1 shows, doctors prescribed opioid analgesics to a higher percentage of white patients than non-white patients at all time points. Compared to white patients, black patients were 36% less likely to receive an opioid analgesic for pain than white patients, Hispanics were 31% less likely and Asians were 27% less likely1. To offset the differences in the prescribing of opioid analgesics doctors prescribed non-opioid analgesics at a higher rate for non-white (32%) than white (26%) patients.
There are several limitations to this study worth discussing. First, the NHAMCS does not include substantial clinical information. Specifically, the survey does not ask if the patient requested an opioid, the ability of patients to pay for a prescription, or in what quantity the doctor prescribed the opioid. Second, the survey instrument does not record information about drug and alcohol abuse or dependency. Lastly, hospital staff might have misclassified participant’s race/ethnicity because survey data is based on recording of staff perception of participant’s race/ethnicity rather than the participant’s self-report of race/ethnicity.
Although overall rates of opioid prescribing for pain have increased since hospitals implemented the JCAHO standards of care in 2001, a discrepancy in the rates of opioid prescribing between whites and other races and ethnicities remained constant throughout the study period. Although it is possible that the discrepancy highlighted in this study is due to an over-prescribing among white-patients who abuse opioids, this does not appear to be the case because researchers found the same discrepancy in children, who are unlikely to be abusing opioids. These results suggest a true racial/ethnic bias among healthcare providers is involved and indicate that JCAHO and other health advocates will need to do more to decrease disparities in health care. To attempt to explain discrepancies in doctors’ prescribing for pain relief, future versions of the NHAMCS could include information about patients’ alcohol and drug history, opioid prescribing history, and awareness of medical options to treat pain.
What do you think? Please use the comment link below to provide feedback on this article.
________________
[1] Adjusted for age, sex, insurance, type of pain, cancer diagnosis, alcohol intoxication/withdrawal/abuse, alcohol dependence, drug intoxication/withdrawal/abuse, drug dependence, hospital location, owner and setting, and survey year.
References
Chapman, C. R. (2000). New JCAHO Standards for Pain Management: Carpe Diem! APS Bulletin Retrieved January 24, 2008, from http://www.ampainsoc.org/pub/bulletin/jul00/pres1.htm
National Center for Health Statistics. (2006). Health. Hyattsville, MD: CDC.
Pletcher, M. J., Kertesz, S. G., Kohn, M. A., & Gonzales, R. (2008). Trends in opioid prescribing by race/ethnicity for patients seeking care in US emergency departments. Journal of the American Medical Association, 299(1), 70-78.
Stewart, W. F., Ricci, J. A., Chee, E., Morganstein, D., & Lipton, R. (2003). Lost productive time and cost due to common pain conditions in the US workforce. Journal of the American Medical Association, 290(18), 2443-2454.
Tamayo-Sarver, J. H., Hinze, S. W., Cydulka, R. K., & Baker, D. W. (2003). Racial and ethnic disparities in emergency department analgesic prescription. American Journal of Public Health, 93(12), 2067-2073.